Diagnoses We Treat, Including Female Sexual Pain Syndromes, Incontinence, and Other Pelvic Floor Issues
At Femina Physical Therapy, we specialize in treating these conditions that are all too often misunderstood by the medical community. What sets us apart from other physical therapy offices is we provide one-on-one care by licensed physical therapists for 55-120 minutes. In certain circumstances we offer appointments over 2 hours. No unlicensed personnel are used at any time, making the quality of care we provide at the highest level, allowing you to reach your goals…and reach them faster.
In depth evaluations, manual therapy, exercise prescription, and many of the other services we offer will have their greatest impact on your recovery when done by skilled, licensed providers that also participate in ongoing continuing education. This practice model also allows us to quickly identify when changes in your treatment plan are needed, maximizing each treatment session. Make an appointment at one of our offices today to get on the path to healing tomorrow.
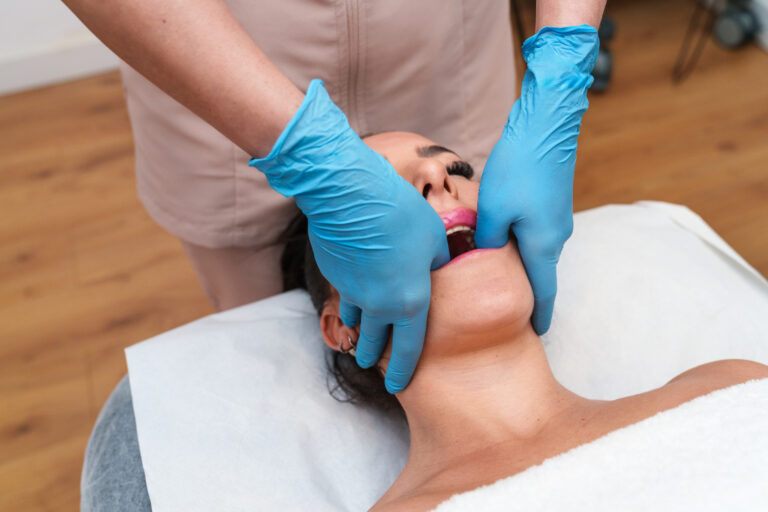
TMJ Dysfunction – Jaw Pain, Headaches, and Therapy Approaches
TMJ Dysfunction – Jaw Pain, Headaches, and Therapy Approaches Jaw pain, recurring headaches, and facial discomfort often stem from dysfunction of the temporomandibular joint (TMJ).

Abdominal Phrenic Dyssynergia: Causes of Bloating and Treatment Approaches
Abdominal Phrenic Dyssynergia: Causes of Bloating and Treatment Approaches Abdominal bloating is a common yet often misunderstood condition, affecting individuals across various demographics. While bloating

Dyspareunia (Painful Intercourse): Symptoms and Treatment Pathways
Dyspareunia (Painful Intercourse): Symptoms and Treatment Pathways Intimacy should be a source of connection, pleasure, and closeness—but for many women, it becomes a source of

Post-Surgical Conditions: Healing, Mobility, and Treatment Options
Post-Surgical Conditions: Healing, Mobility, and Treatment Options Recovering from post-surgical conditions can be a challenging journey—physically, mentally, and functionally. While the surgeon’s work is critical,

Painful Bladder Syndrome / Interstitial Cystitis – Managing Bladder Pain and Restoring Function
Painful Bladder Syndrome / Interstitial Cystitis – Managing Bladder Pain and Restoring Function Living with constant bladder discomfort, urinary urgency, or pelvic pain can be
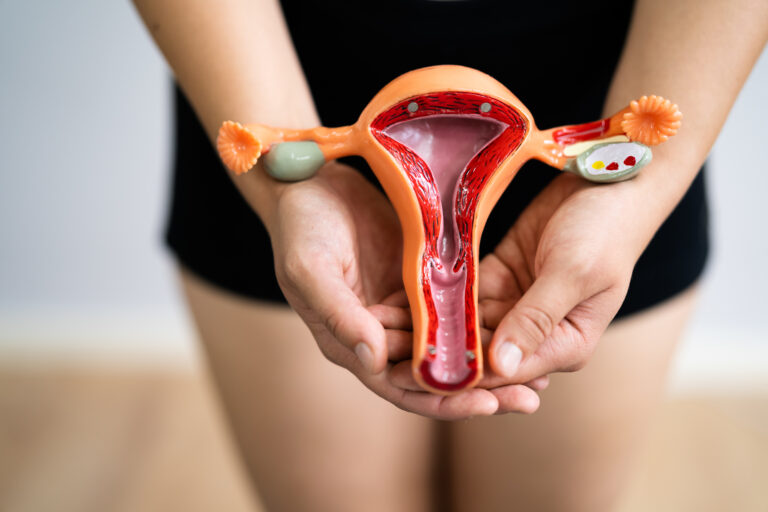
Vulvodynia: Chronic Vulvar Pain Causes, Symptoms, and Treatment
Vulvodynia: Chronic Vulvar Pain Causes, Symptoms, and Treatment For countless women, vulvar pain is a hidden struggle. It may appear as a constant burning, a

Menopause – Common Symptoms and Physical Therapy Approaches
Menopause – Common Symptoms and Physical Therapy Approaches Menopause marks a major transition in a woman’s life, often accompanied by physical, emotional, and functional changes.

Cancer Rehabilitation: Restoring Function and Improving Quality of Life
Cancer Rehabilitation: Restoring Function and Improving Quality of Life A cancer diagnosis and its treatments (surgery, radiation, chemotherapy, hormone therapy) can affect more than just

Endometriosis-Related Pelvic Pain: How Physical Therapy Can Help
Endometriosis-Related Pelvic Pain: How Physical Therapy Can Help Endometriosis is a chronic condition that often brings with it substantial and sometimes debilitating pelvic pain. Many

Orthopedic Conditions & Low Back Pain: Symptoms, Treatment, and Rehabilitation
Orthopedic Conditions & Low Back Pain: Symptoms, Treatment, and Rehabilitation Orthopedic conditions and low back pain affect millions of women worldwide and are among the

Constipation & Dyssynergic Defecation: Types of Bowel Dysfunction and Treatment
Constipation & Dyssynergic Defecation: Types of Bowel Dysfunction and Treatment Constipation is one of the most common digestive and pelvic floor complaints, yet it’s often

Pudendal Neuralgia: Nerve Pain in the Pelvis and How It’s Treated
Pudendal Neuralgia: Nerve Pain in the Pelvis and How It’s Treated Pudendal neuralgia is a debilitating condition characterized by chronic pelvic nerve pain, often caused

Pregnancy & Postpartum: Common Conditions, Recovery, and Treatment Options
Pregnancy & Postpartum: Common Conditions, Recovery, and Treatment Options Pregnancy and the postpartum period are transformative phases in a woman’s life, bringing both joy and

Urogenital & Pelvic Organ Prolapse: What It Is, Symptoms, and How Physical Therapy Can Help
Urogenital & Pelvic Organ Prolapse: What It Is, Symptoms, and How Physical Therapy Can Help Pelvic organ prolapse is a common yet often misunderstood condition

Incontinence: Types, Causes, Symptoms, and Treatment Options
Incontinence: Types, Causes, Symptoms, and Treatment Options Incontinence, or the involuntary passage of urine or stool, is a condition that affects millions of people worldwide.

Female Sexual Dysfunction and Chronic Pain Syndromes
Female Sexual Dysfunction and Chronic Pain Syndromes Female sexual pain syndromes causing painful intercourse can occur for a number of reasons. A high percentage of
Physical Therapy After Pelvic and Breast Cancer
Specialized Physical Therapy after Pelvic and Breast Cancer Treatment Physical therapy for pelvic cancer can relieve pain with sex and general pelvic pain that results

Other Pelvic Floor Issues
Our experience solving a wide range of pelvic floor issues is unmatched in our field, including some less common issues that other therapies cannot always

TMJ Dysfunction – Jaw Pain, Headaches, and Therapy Approaches
TMJ Dysfunction – Jaw Pain, Headaches, and Therapy Approaches Jaw pain, recurring headaches, and facial discomfort often stem from dysfunction of the temporomandibular joint (TMJ).

Abdominal Phrenic Dyssynergia: Causes of Bloating and Treatment Approaches
Abdominal Phrenic Dyssynergia: Causes of Bloating and Treatment Approaches Abdominal bloating is a common yet often misunderstood condition, affecting individuals across various demographics. While bloating

Dyspareunia (Painful Intercourse): Symptoms and Treatment Pathways
Dyspareunia (Painful Intercourse): Symptoms and Treatment Pathways Intimacy should be a source of connection, pleasure, and closeness—but for many women, it becomes a source of

Post-Surgical Conditions: Healing, Mobility, and Treatment Options
Post-Surgical Conditions: Healing, Mobility, and Treatment Options Recovering from post-surgical conditions can be a challenging journey—physically, mentally, and functionally. While the surgeon’s work is critical,

Painful Bladder Syndrome / Interstitial Cystitis – Managing Bladder Pain and Restoring Function
Painful Bladder Syndrome / Interstitial Cystitis – Managing Bladder Pain and Restoring Function Living with constant bladder discomfort, urinary urgency, or pelvic pain can be

Vulvodynia: Chronic Vulvar Pain Causes, Symptoms, and Treatment
Vulvodynia: Chronic Vulvar Pain Causes, Symptoms, and Treatment For countless women, vulvar pain is a hidden struggle. It may appear as a constant burning, a

Menopause – Common Symptoms and Physical Therapy Approaches
Menopause – Common Symptoms and Physical Therapy Approaches Menopause marks a major transition in a woman’s life, often accompanied by physical, emotional, and functional changes.

Cancer Rehabilitation: Restoring Function and Improving Quality of Life
Cancer Rehabilitation: Restoring Function and Improving Quality of Life A cancer diagnosis and its treatments (surgery, radiation, chemotherapy, hormone therapy) can affect more than just

Endometriosis-Related Pelvic Pain: How Physical Therapy Can Help
Endometriosis-Related Pelvic Pain: How Physical Therapy Can Help Endometriosis is a chronic condition that often brings with it substantial and sometimes debilitating pelvic pain. Many

Orthopedic Conditions & Low Back Pain: Symptoms, Treatment, and Rehabilitation
Orthopedic Conditions & Low Back Pain: Symptoms, Treatment, and Rehabilitation Orthopedic conditions and low back pain affect millions of women worldwide and are among the

Constipation & Dyssynergic Defecation: Types of Bowel Dysfunction and Treatment
Constipation & Dyssynergic Defecation: Types of Bowel Dysfunction and Treatment Constipation is one of the most common digestive and pelvic floor complaints, yet it’s often

Pudendal Neuralgia: Nerve Pain in the Pelvis and How It’s Treated
Pudendal Neuralgia: Nerve Pain in the Pelvis and How It’s Treated Pudendal neuralgia is a debilitating condition characterized by chronic pelvic nerve pain, often caused

Pregnancy & Postpartum: Common Conditions, Recovery, and Treatment Options
Pregnancy & Postpartum: Common Conditions, Recovery, and Treatment Options Pregnancy and the postpartum period are transformative phases in a woman’s life, bringing both joy and

Urogenital & Pelvic Organ Prolapse: What It Is, Symptoms, and How Physical Therapy Can Help
Urogenital & Pelvic Organ Prolapse: What It Is, Symptoms, and How Physical Therapy Can Help Pelvic organ prolapse is a common yet often misunderstood condition

Incontinence: Types, Causes, Symptoms, and Treatment Options
Incontinence: Types, Causes, Symptoms, and Treatment Options Incontinence, or the involuntary passage of urine or stool, is a condition that affects millions of people worldwide.

Female Sexual Dysfunction and Chronic Pain Syndromes
Female Sexual Dysfunction and Chronic Pain Syndromes Female sexual pain syndromes causing painful intercourse can occur for a number of reasons. A high percentage of
Physical Therapy After Pelvic and Breast Cancer
Specialized Physical Therapy after Pelvic and Breast Cancer Treatment Physical therapy for pelvic cancer can relieve pain with sex and general pelvic pain that results

Other Pelvic Floor Issues
Our experience solving a wide range of pelvic floor issues is unmatched in our field, including some less common issues that other therapies cannot always
