Some patients are surprised to learn what your bowel movements say about your health.
They are in the office to with pelvic floor dysfunction and problems like urinary incontinence or pain with sex - what does that have to do with poop?
Bowel function is a key piece in the journey towards healing from pelvic floor dysfunction. A lot of our clients with pelvic floor dysfunction, pelvic pain, endometriosis, and prolapse have some trouble with their bowels - either constipation, straining, or diarrhea. These bowel-related issues can cause abdominal pain, painful bloating, rectal pain, and pelvic floor problems. It’s a connection that is very important to consider!
Today we will discuss what your bowel movements say about your health and what poop color, texture, and size might be telling you. If you tend to turn your head when you flush, consider taking a look. There are some important details about your health that can be gathered from the color of your poop, so consider taking a gander at your poop before you flush it away.
Color
According to the Mayo Clinic, stool color can vary widely and still be considered normal. Most stool ranges in shades of brown and green. The variance in color is due to what you are eating as well as the amount of bile present in your stool. Bile is the fluid secreted by your gallbladder that digests fats in your GI system. Bile starts out a yellow-green color and slowly changes color from green to brown depending on what other substances are in your GI tract.
If your poop is bright red or black, you may have blood in your stool. If this is the case, go see a doctor.
More information about poop color and what it may tell you can be found in the charts below:
(source: https://www.mayoclinic.org/stool-color/expert-answers/faq-20058080).
Stool quality | What it may mean | Possible dietary causes |
Green | Food may be moving through the large intestine too quickly, such as due to diarrhea. As a result, bile doesn't have time to break down completely. | Green leafy vegetables, green food coloring, such as in flavored drink mixes or ice pops, iron supplements. |
Light-colored, white or clay-colored | A lack of bile in stool. This may indicate a bile duct obstruction. | Certain medications, such as large doses of bismuth subsalicylate (Kaopectate, Pepto-Bismol) and other anti-diarrheal drugs. |
Yellow, greasy, foul-smelling | Excess fat in the stool, such as due to a malabsorption disorder, for example, celiac disease. | Sometimes the protein gluten, such as in breads and cereals. See a doctor for evaluation. |
Black | Bleeding in the upper gastrointestinal tract, such as the stomach. | Iron supplements, bismuth subsalicylate (Kaopectate, Pepto-Bismol), black licorice. |
Bright red | Bleeding in the lower intestinal tract, such as the large intestine or rectum, often from hemorrhoids. | Red food coloring, beets, cranberries, tomato juice or soup, red gelatin or drink mixes. |
Texture
IBS can cause changes in the consistency of stools, usually harder or much softer than usual. At the clinic we use a handy scale called the Bristol Stool Scale to help therapists categorize your poop. The texture of your stool gives you an idea of how much time it has spent in the colon. Factors besides IBS that may affect poop texture include diet, fluid intake, medications, pelvic floor dysfunction, and lifestyle can be factors that play into the texture of your stool as well.
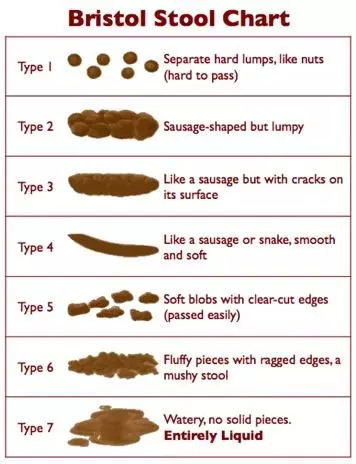
The Bristol Stool Chart shows seven categories of stool, in general:
Types 1-2 may indicate constipation
Types 3-4 indicate ideal stools that are easy to pass
Types 5-7 indicate diarrhea
However, if you are straining to evacuate your stools (pushing, holding your breath, turning your face red, etc.)- go see a pelvic floor therapist as you might be having some pelvic floor issues which might be contributing to your problem.
Size
Irritable bowel syndrome can cause your stools to be smaller, larger or narrower than usual.
According to the Mayo Clinic, if you have pencil thin poops every once in a while, it is probably harmless. However, if your poops are pencil thin for more than 1-2 weeks, it may indicate a narrowing or obstruction of the colon due to colon cancer or a pelvic floor dysfunction.
Other Changes
Consult your doctor immediately if your bowel changes are accompanied by rectal bleeding or severe abdominal pain. Pelvic floor therapy can help you if you are experiencing pelvic pain and voiding issues, so don’t be shy about contacting us if you are concerned by what your bowel movements say about your health.
Resources
Blake, M. R., Raker, J. M., & Whelan, K. (2016). Validity and reliability of the Bristol Stool Form Scale in healthy adults and patients with diarrhoea-predominant irritable bowel syndrome. Alimentary Pharmacology & Therapeutics, 44(7), 693–703.doi:10.1111/apt.13746
Mayo Clinic, Stool color: When to worry Expert Answers from Michael F. Picco, M.D. Accessed on 4/10/19 from:
https://www.mayoclinic.org/stool-color/expert-answers/faq-20058080
Mayo Clinic, Narrow stools: Should I be concerned? Expert Answers from Michael F. Picco, M.D.https://www.mayoclinic.org/narrow-stools/expert-answers/faq-20057781